 Home
Home
August 19, 2025
Considerations for Antiseizure Medication Conversions
Our hospice partners occasionally ask how to convert patients from one antiseizure medication (ASM) to another. These requests are usually driven by cost or formulary considerations, but other common reasons include lack of efficacy, intolerable adverse effects, and problematic drug-drug interactions.
Ideally, formulary / cost shouldn’t be the sole basis for rotating to an alternate ASM, especially since there’s risk of jeopardizing seizure control or negatively impacting quality of life. Newer, often more expensive, ASMs may have superior tolerability, especially in populations vulnerable to ASM toxicity (e.g., older adults).1 ASM regimens are typically chosen after careful consideration, expert consultation, and in some cases numerous drug trials. So, it’s generally recommended to stay the course and avoid ASM conversion in patients whose seizures are well-controlled on drug regimens that are well-tolerated.2
ASM conversions are less straightforward than other drug conversions (e.g., opioids, SSRIs) and warrant a more cautious approach. Experts recommend using a process called transitional polytherapy (Figure 1), where the new ASM is added and gradually titrated to a therapeutic dose before the baseline ASM is tapered and eventually withdrawn.1 Temporarily overlapping the ‘old’ and ‘new’ medications is recommended to minimize the risk of breakthrough seizures or withdrawal effects.
Titrating and tapering strategies have been described for various ASMs (Table 1) and can be used to guide plans for switching.1,3,4 If a patient is experiencing severe adverse effects with their current ASM, it should be tapered more rapidly. More gradual tapering can be considered for patients with poor seizure control. Side effects including sedation, dizziness, fatigue, headache, and ataxia are frequently encountered with ASM use, especially during titration and conversion periods.1 While careful monitoring for adverse effects is routinely recommended when starting new medications, particular care and attention is warranted during transitional polytherapy.
While transitional polytherapy offers a reasonable framework for switching ASMs, the risks, benefits, and timing of these changes must be carefully weighed. In many cases, preserving seizure control and minimizing new side effects will be more important than formulary alignment. ASM conversions in hospice care require more than clinical expertise—they call for a team-based, patient-centered approach. Ultimately, the best ASM regimen is the one that supports patient comfort and aligns with their goals of care.
Figure 1. Transitional Polytherapy Conceptualization
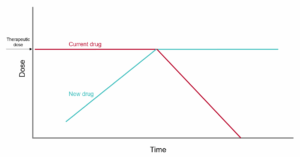
Table 1 Literature-based ASM tapering and titration strategies4,5
| ASM | Tapering | Titration |
|---|---|---|
| Carbamazepine | • Reduce original dose by 20% every 7 days • Faster taper can be considered in hepatic impairment or if converting to oxcarbazepine | • Up to 200mg/day in 2-4 divided doses initially; may increase by 200mg/day every 7 days to usual dose of 400-800mg/day • Faster titration could be considered if converting from oxcarbazepine • Slower titration recommended if elderly, hepatic impairment, or converting from felbamate |
| Felbamate | • Reduce original dose by 25% every 7 days • Faster taper can be considered in hepatic impairment | • Week 1: 1.2g/day in 3-4 doses; reduce dose of existing ASM by 33% • Week 2: Increase felbamate to 2.4g/day; reduce existing ASM by an additional 33% • Week 3: Increase felbamate to 3.6g/day; continue to reduce existing ASM as indicated |
| Gabapentin | • Reduce original dose by 25% every 7 days • Faster taper can be considered in renal impairment | • 600-900mg/day initially; increase by 600-900mg/day every 7 days up to 2400-3600mg/day • Consider slower titration in renal impairment or older adults |
| Lacosamide | • Reduce gradually by up to 200mg/day every 7 days | • 50mg twice daily initially; increase by 50mg twice daily every 7 days to maintenance dose of 100-200mg twice daily |
| Lamotrigine | • Reduce original dose by 20-25% every 7 days • Some experts suggest withdrawing lamotrigine over months • Faster taper can be considered in hepatic impairment or concomitant valproic acid use | • Titration depends on existing ASM; refer to prescribing information |
| Levetiracetam | • Reduce original dose by 20-25% every 7 days • Faster taper can be considered in renal impairment | • 500mg twice daily initially; increase by 500mg/dose up to every 7 days to an initial target dose of 1000-2000mg/day • Consider slower titration in renal impairment or older adults |
| Oxcarbazepine | • Reduce original dose by 20-25% every 7 days • Faster taper can be considered if converting to carbamazepine | • 300-600mg/day in 2 divided doses initially; increase dose by 300mg every 7 days up to target dose of 900-1500mg day • Consider slower titration in hepatic impairment |
| Phenobarbital | • Reduce original dose by 10-25% every month • Faster taper recommended for patients on therapy for <1 month | • 2mg/kg/dose in divided doses initially • Dose should be individualized based on clinical response and serum concentration |
| Phenytoin | • Reduce original dose by 20-25% every 7 days • Faster taper can be considered in hepatic impairment | • 3-5mg/kg/day initially; further • Dose adjustments depend on steady state serum levels |
| Topiramate | • Reduce original dose by 20-25% every 7 days • Faster taper can be considered in renal impairment | • 25-50mg/day initially; increase by 25-50mg/day every 7 days up to 100-200mg/day • Consider slower titration / smaller dose increase in renal impairment or older adults |
| Valproic acid and derivatives | • Reduce original dose by 20-25% every 7days • Faster taper can be considered in hepatic impairment | • 500-1000mg/day initially; increase by 250-750mg/day every 7 days up to 1000-2000mg/day • Dose adjustments may be guided by serum levels • Consider smaller dose increase in elderly • Slower titration may reduce nausea |
| Zonisamide | • Reduce original dose by 20-25% every 7 days | • 100mg/day initially; increase dose by 100mg every 2 weeks up to target dose of 300-400mg/day |
Written by: OnePoint Patient Care Clinical Team
References
- St. Louis E. The Art of Managing Conversions between Antiepileptic Drugs: Maximizing Patient Tolerability and Quality of Life. J Pharmaceuticals. 2010;3(9):2956-2969. doi: 10.3390/ph3092956
- Jobst B, Holmes G. Prescribing Antiepilectic Drugs: Should Patients Be Switched on the Basis of Cost? CNS Drugs. 2004; 18(10):617-628. doi: 216/0023210-200418100-00001
- Garnett W, St. Louis E, Henry T, Bramley T. Transitional Polytherapy: Tricks of the Trade for Monotherapy to Monotherapy AED Conversion. Current Neuropharmacology. 2009;7(2):83-95. doi: 2174/1570159097884884
- Louis E, Gidal B, Henry T, et al. Conversions between monotherapies in epilepsy: Expert Consensus. Epilepsy Behav. 2007;11(2):222-234. doi: 10.1016/j.yebeh.2007.04.007
- Lexicomp Online, Lexi-Drugs Online, Hudson, Ohio: Wolters Kluwer Clinical Drug Information, Inc.; 2024.